An anal abscess, an infected wound that drains pus from your anus, is typically the cause of an anal fistula. The draining abscess may potentially tunnel to the skin outside of your anus. The main symptoms are redness, swelling, and soreness in the anal area. Surgery is the primary therapeutic option.
Overview
What is an anal fistula?
An anal fistula is an uneven tube that develops from the inside of your anus to the skin outside of it. It usually appears in the upper part of your anus, or butthole, where your anal glands are situated. When these glands get polluted, the infection’s discharge may result in the development of a fistula. This illness is known as a perianal abscess. (Perianal fistulas is another term that is occasionally used to describe anal fistulas. “Perianal” denotes the region surrounding your anus.)
How common is this condition?
One somewhat common anorectal ailment is a fistula. It is twice as likely to occur in men and those classified as male at birth (AMAB). About half of patients with an infected anal gland develop a fistula. 75% of anal fistula are caused by an infected gland that produces an abscess, a pocket of pus that has to drain.
Symptoms and Causes
What are anal fistula symptoms?
These are the most typical signs of an anal fistula:
1. Anal pain, frequently throbbing and strong. You may feel it more when you sit, cough, or poop. It’s possible that you can feel your butt.
2. irritation and redness in or around your anus. These signify the presence of a live cellulitis infection under the skin.
3. Fluid dripping from your anus in some areas. It could consist of blood (rectal hemorrhage), pus, or feces. It might be smelling.
Less common symptoms include:
1. Pain when you pee.
2. Fever.
3. Difficulty holding your poop in.
Using a mirror, you might or might not be able to view the fistula.
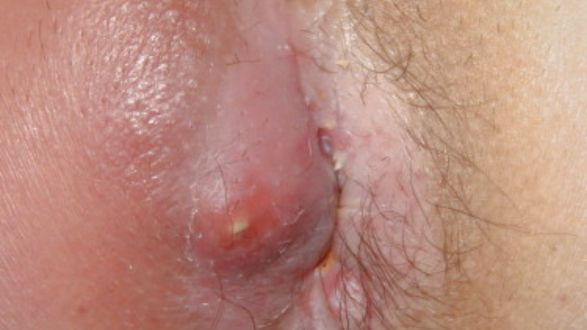
What does an anal fistula look like?
An anal fistula appears as a hole in the skin near your anus. The outermost portion of the tunnel leading to the internal abscess is actually the hole. It may leak discharge, especially if you come into contact with pus, blood, or excrement on the surrounding skin. Some older fistulas may seal at the opening, while the remainder of the tunnel remains open. This causes pain and swelling until the fistula reopens to discharge the drainage.
What is the main cause of a fistula?
Fistulas can develop anywhere in your body, from one organ to another or from one organ to a skin incision. They typically appear after an injury or illness causes your tissues to become inflamed for an extended period of time. Persistent infection and inflammation, particularly when pus needs to drain, might eventually erode into the surrounding tissues. This may open a passageway between the surrounding tissues and the wound.
What causes an anal fistula?
Anal gland infection is typically the site of a perianal abscess, which is the most frequent cause of an anal fistula. A pocket of pus that forms at the site of an infection is called an abscess. The pus must escape, and it might make a channel for itself to do so. To treat an abscess, a medical professional may occasionally build a drainage route. However, the wound frequently does not heal entirely, leaving a fistula. The following are uncommon causes of anal fistula:
1. Gastrointestinal disorders that cause inflammation, such as Crohn’s disease.
2. Anal STIs (sexually transmitted infections).
3. Tuberculosis affecting your anus.
4. A severe wound or prior surgery to your anus.
5. Treatment with radiation for pelvic cancer.
6. Actinomycosis is an uncommon bacterial illness that can occasionally result in perianal abscesses.
7. Chronic inflammatory skin illness called hidradenitis suppurativa can cause abscesses in your sweat glands and sometimes in your perianal area.
Which variables put one at risk of developing an anal fistula?
An anal fistula is more likely to occur if you:
1. Were assigned male at birth.
2. Possess or have previously had a perianal abscess.
3. Possess a Crohn’s-like inflammatory bowel disease (IBD).
4. own a medical history of radiation treatment or surgery in your perianal area.
5. Possess weakened immune systems or are more vulnerable to illnesses.
6. Have a chronic STI.
What consequences could an anal fistula cause?
If left untreated, a fistula usually won’t repair itself. Long-term issues like the following could result from this:
1. Persistent infection: An abscess or infection may remain active if a fistula results from it. The infection may appear to disappear at the initial location and then reappear, creating a fresh abscess and producing excruciating pain. At times, the fistula may appear to be healing and shut at the opening, but then it may reopen due to recurrent infection and drainage.
2. Fistula extension: Rarely, a chronic fistula may grow in new directions, resulting in new skin holes and branching channels. Repairing these intricate fistulas is extremely challenging.
3. Cancer: Anal fistulas that have been there for years might sometimes be linked to anal cancer. Erosion and persistent inflammation are recognized as cancer risk factors.
Diagnosis and Tests
How is an anal fistula diagnosed?
The majority of anal fistulas are detectable by medical professionals by physical examination, yet occasionally the external opening closes. Additionally, your physician will search for the fistula’s internal entrance within your anus. This section may need to be sedated. Your healthcare professional might have to examine you under sedation in the operating room if touching or opening your anus causes excessive pain.
Your healthcare professional may use a lighted scope, such as an anoscope or proctoscope (a larger scope that can visualize your rectum), to locate the internal cause of the fistula. To identify the infection at the fistula’s origin, medical professionals occasionally inject hydrogen peroxide into the external aperture. When the peroxide and infection interact, foam or bubbles are produced at the location. The fistula can be confirmed by locating the internal source.
Will I have any other medical tests?
It may be necessary for your healthcare professional to perform (Radiological) tests to track the course of your fistula. This could imply:
1. MRI (magnetic resonance imaging): A high-detail, non-invasive imaging exam is an MRI. This can assist medical professionals in charting the tunnel’s course and determining how it affects your muscles and other organs.
2. Endoscopic ultrasound: Endoscopic ultrasound uses a tiny illuminated camera and a tiny ultrasonic probe to create images inside your abdomen instead of an MRI, which creates images comparable to what it sees.
3. Fistulography: Your healthcare professional will take an X-ray of your fistula after injecting dye into it, which is known as a fistulogram. The fistula’s route will be highlighted by the dye.
Your physician has to know the course of treatment for your fistula to make that decision. Your fistula will be categorized based on its course.
What are the different types of anal fistulas?
Anal fistulas are categorized by medical professionals based on how close they are to your anal sphincter muscles. Your bowel movements are controlled by these muscles, therefore it’s critical to maintain their health. Depending on where it is located, your provider may refer to your anal fistula by a particular name, like:
1. Intersphincteric anal fistula: Burrows out via the area between your internal and external sphincter muscles after passing through your internal anal sphincter muscle.
2. Transsphincteric fistula: Passes past the anal sphincter muscles’ two layers.
3. Suprasphincteric fistula: Circumvents your external sphincter after passing past your internal sphincter.
4. Extrasphincteric fistula: Circumvents the two sphincter muscles. This less common form normally starts from your rectum rather than your anus, and it is not from the anal gland.
5. Superficial anal fistula: Passes through the surrounding skin from the bottom portion of your anal canal, beneath your anal glands, and avoids using your muscles. This kind is not derived from the anal gland.
The sort of anal fistula you have doesn’t need to be known to you, but it will affect how your healthcare provider manages it. If a large portion of your sphincter muscles are involved, the course of treatment may need to be changed. When surgeons repair your anal fistula, they must take care to avoid hurting these muscles.
Management and Treatment
What is the treatment for an anal fistula?
Surgery is usually required to repair anal fistulas. After spontaneous healing, the fistula often reopens due to recurrent infections and abscesses. On the other hand, if your fistula is uninfected and the result of inflammatory bowel illness, it may occasionally heal with medical intervention. In order to treat these fistulas, your doctor may first attempt immunomodulator therapy, such as infliximab.
Surgery
Depending on how simple or complicated the fistula is, anal fistula surgery can be either simple or complex. Simple, intersphincteric fistulas that only involve a short bit of muscle are the most prevalent type of anal fistulas. Treating these with a single procedure is safe. Stepwise surgery may be required for more difficult fistulas.
1. Simple fistulas: Your anal fistula is regarded as uncomplicated if it just includes a small amount of muscle and has no branches. The surgical treatment performed to treat a simple fistula is called a fistulotomy. About 95% of patients find that this one-step operation is the most straightforward and successful technique to cure an anal fistula.
2. Fistulotomy: The fistula’s roof will be sliced through by your colorectal surgeon to allow it to fill in from the bottom up. They may also take out tissue that is contaminated. A small amount of muscle may be cut when cutting through the roof, but that’s okay. If you make too many muscle cuts, your bowel control may suffer.
Complex fistulas
If there are branches, a large amount of muscle involved, or if you have underlying medical issues that increase your risk of surgical complications, your fistula is classified as complex. Multiple procedures may be necessary to repair complex fistulas. One or more of these methods may be employed by your colorectal surgeon:
1. Seton drain: One kind of surgical thread that needs to be removed is called a seton since it doesn’t absorb over time. To assist in keeping your fistula open long enough to drain out all of the effluent, a surgeon loops the seton through it. In addition, a seton can gradually sever the fistula tract, allowing the tissue to mend as it penetrates the muscle. Finally, it aids in the localized scarring of the tissue to prevent the incision from rupturing later. Afterward, your surgeon might perform a fistulotomy or similar treatment to remove the drain and seal the fistula. Your surgeon may decide to leave the Seton drain in place forever if a persistent ailment, such as inflammatory bowel disease, is the cause of your fistula.
2. Endorectal advancement flap: By avoiding cutting into the fistula’s ceiling, this treatment preserves the integrity of your sphincter muscles. Rather, the contaminated tissue surrounding the internal hole of your anal fistula is excised by your surgeon. Subsequently, a flap of healthy tissue from the interior of your rectum is pulled down to conceal this opening. After draining from the external opening, the fistula should start to mend from the inside out. Although this operation is thought to be roughly 70% effective, the infection and fistula might nevertheless recur in certain individuals. When cutting the flap, there is still a chance (about 30%) of hurting the sphincter muscle.
3. LIFT procedure: “Ligation of Intersphincteric Fistula Tract” is what LIFT stands for. This refers to the closure (ligation), usually with stitches, of the intersphincteric fistula, which runs between the two sphincter muscles. Next, your surgeon may either scrape away the contaminated tissue within or remove the entire fistula tract from this area. This procedure typically follows a seton drain surgery. It doesn’t run the risk of damaging your sphincter muscles, however, it is marginally less effective than fistulotomy (75%).
What are the risks of anal fistula surgery?
The main risks are:
1. Recurring infection: Should the infection persist within your healing fistula, it might not have entirely disappeared from your fistula. Recurrent infections are often treated with antibiotics.
2. Recurring fistula: An anal fistula may reoccur if surgery is performed and it does not heal completely. This could be the result of the procedure employed, or it could be the result of underlying chronic illnesses.
3. Fecal incontinence: Following anal fistula surgery, some patients have mildly disturbed fecal continence. For instance, individuals may experience some fecal leaks or struggle to hold in gas. More skilled colorectal surgeons see fewer of these problems.
What is recovery like from anal fistula surgery?
Although some patients may need to return for additional surgery down the return, anal fistula operations are typically performed as outpatient procedures, allowing you to return home the same day. You will receive guidelines for self-care as well as prescription painkillers to take home. These could consist of:
1. Water and fiber supplements: Your doctor may recommend fiber supplements to avoid constipation as a side effect of painkillers. It’s crucial to take these along with plenty of water.
2. Sitz bath: At least once a day, soaking your anus in a warm, shallow bath will assist to relieve discomfort and hasten healing.
3. Wound management: In order to keep your wound clean, you might need to use dressings to collect drainage and change them frequently.
Outlook / Prognosis
When I have an anal fistula, what can I anticipate?
Depending on how simple or complex your anal fistula is, your prognosis will change. This establishes the length of the rehabilitation and treatment plan. Generally speaking, recuperating from one or more procedures should take three to six weeks. After surgery, some fistulas recur, particularly if they were caused by a persistent disease or had several branches. Anal fistulas can occur several times in IBD patients.
Living With
What is the appropriate time to see a doctor about an anal fistula?
Consult a doctor whenever you have anal pain. Significantly painful anorectal disorders may be dangerous. Never presume that it will go away on its own. Although they are more prevalent and well-known, hemorrhoids typically don’t hurt all that much. If your pain persists after a general practitioner (primary care) diagnoses you with a hemorrhoid, consult a specialist such as a gastroenterologist or colon surgeon.
Additional Common Questions
What is a perianal vaginal fistula?
Because a perianal vaginal fistula typically links from your rectum to your vagina, it is also known as a rectovaginaginal fistula. The section of your large intestine that comes directly before your anus is called your rectum. Your vagina and rectum share a significantly thinner border than your vagina and anus. Though it typically originates from the colon or rectum, a vaginal fistula can form from any area of your intestines.
What difference distinguishes an anal fistula from an anal fissure?
A split or tear in the anal canal lining is called an anal fissure. A fissure is a superficial wound, yet it can induce symptoms that are similar to those of an anal fistula. Unlike a fistula, it does not burrow through your anal wall to reach your skin. An anal fistula could, nevertheless, grow out of an anal fissure. An anal fistula may result from the draining of an abscess that develops from an infected anal fissure.
A note from Blogjug
Severe anal pain can have crippling effects on one’s body and mind. Not only does it trouble you every time you sit or use the restroom, but talking about it with a healthcare professional may also feel overwhelming. This shouldn’t deter you. Anorectal disorders and diseases are as worthy of attention as any other. Treatment for an anal fistula is necessary, and it will probably be easier the earlier you receive it.









5 thoughts on “Anal Fistula: What It Is, Symptoms, Surgery and Treatment”