Chronic Pain
All areas of the body experience chronic pain, which can endure for months or even years. It disrupts day-to-day activities and may result in anxiety and sadness. Identifying and treating the cause is the first stage in treatment. The best course of action is to combine medication, therapy, and lifestyle modifications when that isn’t feasible.
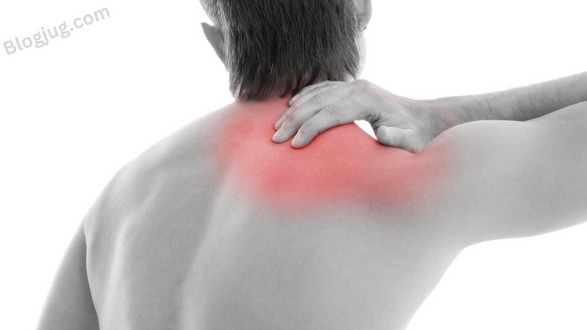
Overview
What is chronic pain?
Chronic pain is defined as any discomfort that persists for more than three months. The pain may never go away or it may just occasionally occur. It could occur somewhere in. your body
Your everyday activities, including working, socializing, and taking care of others or yourself, may be hampered by chronic pain. It can worsen your discomfort by causing anxiety, despair, and difficulty sleeping. This response sets off an extremely difficult-to-break vicious cycle.
What difference between other pain and chronic pain?
Acute and chronic pain are two different categories of pain. When you are injured, such as by a little cut on your skin or a shattered bone, you experience acute agony. The discomfort subsides quickly after your body recovers from whatever triggered it. On the other hand, chronic pain persists long after a sickness or injury has healed. It even occurs occasionally for no apparent cause.
Where do people have chronic pain?
There are numerous ways that chronic pain can manifest itself throughout your body. Common forms of long-term pain include:
1. Back pain.
2. Arthritis, or joint pain.
3. Neck pain.
4. Cancer pain near a tumor.
5. Headaches, including migraines.
6. Testicular pain.
7. Muscle pain all over.
8. Pain that persists in scar tissue.
9. Damage to the nerves or other components of the nervous system can result in neurogenic pain.
How common is chronic pain?
One of the most frequent conditions for which people seek medical attention is chronic pain. In the US, almost 25% of adults report having chronic pain.
Symptoms and Causes
What causes chronic pain?
Occasionally there is a clear reason for chronic pain. You can be experiencing chronic pain from a chronic illness like cancer or arthritis.
Your body may alter as a result of illnesses or injuries, making you more sensitive to pain. Even after the initial illness or injury has healed, these alterations may persist. You could have chronic pain from a sprain, broken bone, or transient infection.
Additionally, some persons experience persistent pain that is unrelated to a medical condition or injury. Physicians refer to this reaction as psychogenic or psychosomatic pain. Psychological elements including stress, worry, and depression are the root cause of it. Many scientists think that reduced blood levels of endorphins are the cause of this link. Natural molecules called endorphins are known to elicit happy emotions.
It is feasible for many pain causes to coexist. For instance, you can be suffering from two distinct illnesses. Alternatively, you might experience both psychogenic pain and migraines.
What does chronic pain feel like?
Individuals who experience chronic pain can express it in a variety of ways, including:
1. Stiffness.
2. Stinging.
3. Throbbing.
4. Aching.
5. Burning.
6. Shooting.
7. Squeezing.
Other symptoms and illnesses that are frequently brought on by chronic pain include:
1. Depression.
2. Anxiety.
3. Mood swings.
4. Fatigue, or the constant state of being excessively exhausted.
5. Insomnia, and trouble falling asleep.
Diagnosis and Tests
How is chronic pain diagnosed?
If pain persists or fluctuates (recurs) for longer than three months, it is deemed chronic. Since pain is typically a symptom, your healthcare professional should try to identify the source of your discomfort. Because pain is subjective and only the individual experiencing it can define and recognize it, diagnosing the cause can be challenging for healthcare professionals.
Consult your healthcare practitioner if your pain is persistent. What your provider needs to know is:
1. Where is your pain?
2. On a range of 0 to 10, How intense is it?
3. How frequently it happens?
4. How much of an impact it has on your life and work?
5. Who improves or deteriorates it?
6. Whether your life is filled with a great deal of tension or anxiety.
7. Whether medical conditions or operations you’ve had.
Which examinations are performed to identify chronic pain?
To find the source of your discomfort, your healthcare professional may do physical examinations and prescribe certain tests. You might be required to take the following tests:
1. Blood tests.
2. To measure muscle activity, use electromyography.
3. Imaging tests including MRIs and X-rays.
4. Nerve conduction testing to determine the appropriate response of your nerves.
5. Tests of balance and reflexes.
6. Urine tests.
8. Spinal fluid tests.
Management and Treatment
How is chronic pain treated?
Healthcare professionals initially attempt to determine and address the source to relieve chronic pain. But occasionally, they are unable to locate the source. In that case, they focus on managing or treating the pain.
Numerous approaches are used by medical professionals to address chronic pain. The strategy is dependent on numerous elements, such as:
1. The type of pain you have.
2. Your pain’s cause, if it is known.
3. Your general health and age.
The most effective treatment programs combine several tactics, including prescription drugs, dietary adjustments, and counseling.
In addition to seeking therapy for your chronic pain, it’s critical to address any co-occurring mental health conditions, such as depression or anxiety. Anxiety or sadness may exacerbate your chronic pain. For instance, the weariness, altered sleep patterns, and potential decrease in activity that come with depression might exacerbate chronic pain.
What medications can treat chronic pain?
Your physician might suggest any of the following drugs to treat chronic pain:
1. Anticonvulsants for nerve pain.
2. Tricyclic antidepressants are examples of antidepressants.
3. Corticosteroid.
4. Muscle relaxers.
5. Medical marijuana.
6. Acetaminophen or nonsteroidal anti-inflammatory medications (NSAIDs).
7. Topical medications (used topically) that have an analgesic or ingredients that create soothing heat or cold.
8. Sedatives to treat sleeplessness or anxiety.
Your doctor may also recommend that you try the following other medical treatments:
1. Transcutaneous electrical nerve stimulation (TENS): Small shocks are applied to your skin through patches during this process. There is pain relief from the electrical impulses.
2. Nerve blocks: To lessen pain perception in the affected location, your healthcare practitioner will inject an anesthetic there. Sometimes, nerve blocks might help identify the source of your pain and offer diagnostic information.
3. Epidural steroid injections: To address chronic pain brought on by irritation and inflammation of the spinal nerve roots, an anti-inflammatory medication injection, either a steroid or a corticosteroid, is administered into the epidural space, which is the region around your spinal nerves.
Does medical treatment for chronic pain have any adverse effects or complications?
There is always a chance of side effects with medications, some of which are more dangerous than others. Make sure you talk to your healthcare provider about any potential adverse effects of the medications you take for chronic pain.
Among the side effects of receiving medical care for chronic pain are:
1. Acute liver failure brought on by taking acetaminophen.
2. Addiction to opioids and/or overdose.
3. Medication-induced mood swings, disorientation, and breathing problems related to nerve pain.
4. Infection or injury to the spinal cord caused by spinal cord stimulators.
Can modifying one’s lifestyle assist with chronic pain?
Four main lifestyle elements might impact and lessen your chronic pain. These are referred to as the four pillars of chronic pain by medical professionals. Among them are:
1. Stress: Reducing stress as much as possible is vital because it can play a significant influence in chronic pain. While everyone manages stress differently, some common strategies include deep breathing, mindfulness, and meditation. Experiment until you find the solution that best suits your needs.
2. Exercise: Engaging in low-impact physical activities, such as strolling or gentle swimming, for half an hour each day could potentially alleviate your discomfort. For some people, exercise also serves as a stress reliever, which is something you should control if you have chronic pain.
3. Diet: Eating a nutritious diet is essential to improving your general health. Your doctor could advise you to follow an anti-inflammatory diet that involves avoiding foods like red meat and processed carbs that aggravate inflammation.
4. Sleep: Your general health depends on getting enough good sleep. You may gain weight as a result of sleep deprivation, which could exacerbate your chronic discomfort. Managing stress also requires getting enough good sleep.
Talk to your healthcare practitioner about these four lifestyle pillars to find out how each relates to your particular form of chronic pain and how you might make adjustments in your day-to-day activities.
Can therapy help with chronic pain?
You may be able to control your chronic pain with the following therapies:
1. Cognitive-behavioral therapy (CBT): This counseling approach teaches you coping mechanisms and helps you view pain from a different perspective.
2. Counseling: You can manage chronic pain, especially psychogenic pain, with the aid of talk therapy.
3. Occupational therapy: Occupational therapy helps you learn new ways to perform daily tasks so that you can minimize pain or prevent injuries.
4. Physical therapy: Exercises used in physical therapy include strengthening and extending your body to assist lessen discomfort.
What other options are there for treating persistent pain?
Alternative therapies that have been demonstrated to gradually reduce chronic pain include:
1. The use of tiny points strategically placed throughout the body in acupuncture.
2. Aromatherapy makes use of essential oils and fragrant herbs.
3. Hypnotherapy, or hypnosis.
4. Training in mindfulness, which teaches you how to relax.
5. Music, art, or pet therapy.
6. Your body’s energy fields can be altered by a therapist utilizing touch in Reiki or Healing TouchTM.
7. Methods of relaxation include massage, mindfulness, and guided imagery.
Is there a cure for chronic pain?
Other than determining and treating its cause, there is currently no cure for chronic pain. For instance, joint pain may occasionally be relieved by treating arthritis.
Many persons with chronic pain are unable to get relief and are unaware of what causes it. To reduce pain, they combine treatments, medicine, and lifestyle modifications.
Prevention
What are the risk factors for chronic pain?
There are various risk factors for developing chronic pain because it can be brought on by a variety of illnesses or injuries. Among the risk factors are:
1. Your genetics: Certain causes of persistent pain, such as migraines, are inherited and run in families.
2. Having obesity: Since obesity puts additional strain on your joints, it can exacerbate certain painful medical problems, such as arthritis.
3. Your age: Arthritis and neuropathy are two conditions that can cause chronic pain in older adults.
4. Having a previous injury: You have an increased risk of developing chronic pain later in life if you have a traumatic injury.
5. Having a labor-intensive job: You run a higher risk of chronic discomfort if you work physically demanding jobs.
6. Experiencing stress: Research has indicated a correlation between regular stress post-traumatic stress disorder and chronic pain.
7. Smoking: Smoking increases your chance of getting sick and necessitates the need for therapy for chronic discomfort.
Can chronic pain be prevented?
Regretfully, there is no known way to stop chronic pain in general. There are some illnesses you might be able to avoid that result in chronic pain. For instance, you can reduce your chance of lung cancer by giving up smoking.
Outlook / Prognosis
What is the outlook (prognosis) for individuals suffering from chronic pain?
Although chronic pain seldom goes away, you can manage it by combining several techniques that are effective for you. Approximately 30% less pain can be experienced by a person using current chronic pain medications.
Researchers are still looking into pain illnesses. Improved knowledge of the human body and developments in neuroscience should result in more potent therapies.
You should get mental health care if you have anxiety, depression, or persistent pain. If left untreated, anxiety and depression can worsen your symptoms and reduce your quality of life even further.
What are the complications of chronic pain?
Chronic pain complications can include:
1. Depression.
2. Anxiety.
3. Substance abuse disorders.
4. Exacerbation of pre-existing chronic illness.
5. A higher chance of suicide or suicidal thoughts.
6. Decreased quality of life.
Serious consequences can arise from prolonged pain. You must get medical attention if you are suffering from persistent discomfort as a result. Pain management and treatment options are many. Finding the ideal mix of therapies that work for you may take some time, but the effort is worthwhile.
Dial 988 to reach the Suicide and Crisis Lifeline if you are thinking about ending your life. You will be able to speak with someone every single day.
Living With
How can I cope with chronic pain?
In addition to changing your lifestyle, having treatment, and taking medication, look after yourself. You can enhance your general health and manage your chronic pain by doing the following steps:
1. Avoid smoking.
2. At a healthy diet.
3. Exercise regularly.
4. Get enough sleep.
5. Manage your stress.
6. Try not to overextend yourself. Make a daily plan with a few priorities and time set aside for relaxation and self-care.
7. Join a chronic pain support group to hear from others dealing with similar issues.
8. Try to think positively.
9. Restrict alcohol consumption as it might exacerbate pain and sleep issues.
What questions should I ask my doctor?
It could be beneficial to ask your healthcare professional the following questions if you experience persistent pain:
1. What’s causing my pain?
2. Will it go away? If not, why not?
3. Which kinds of drugs am I able to take? What adverse consequences do they have?
4. Do I need to try counseling—psychological or physical?
5. Is it safe to exercise?
6. Should I call you if it gets worse?
A note from Blogjug
Months or years can pass between episodes of chronic pain that limit your ability to work, engage in activities, and take care of others or yourself. Please see a doctor or pain specialist if you experience chronic pain. To assist you live a more comfortable life, there are strategies to help you manage your pain.









6 thoughts on “Coping with Chronic Pain: Strategies for Relief”